What is glaucoma?
Glaucoma is a disease of the optic nerve — the part of the eye that carries the images we see to the brain. The optic nerve is made up of many nerve fibers, like an electric cable containing numerous wires. When damage to the optic nerve fibers occurs, blind spots develop. These blind spots usually go undetected until the optic nerve is significantly damaged. If the entire nerve is destroyed, blindness results.
Early detection and treatment by your ophthalmologist (Eye M.D.) are the keys to preventing optic nerve damage and blindness from glaucoma.
Glaucoma is a leading cause of blindness in the United States, especially for older people. But loss of sight from glaucoma can often be prevented with early treatment.
What causes glaucoma?
Clear liquid called aqueous humor circulates inside the front portion of the eye. To maintain a healthy level of pressure within the eye, a small amount of this fluid is produced constantly while an equal amount flows out of the eye through a microscopic drainage system. (This liquid is not part of the tears on the outer surface of the eye.)
Because the eye is a closed structure, if the drainage area for the aqueous humor — called the drainage angle — is blocked, the excess fluid cannot flow out of the eye. Fluid pressure within the eye increases, pushing against the optic nerve and causing damage.
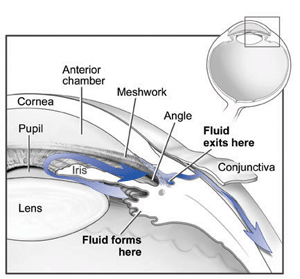
Clear liquid called aqueous humor is constantly being
produced within the eye (left). If the drainage angle of the
eye is blocked, fluid cannot flow out of the eye (right).
What are the different types of glaucoma?
Chronic open-angle glaucoma: This is the most common form of glaucoma in the United States.
The risk of developing chronic open-angle glaucoma increases with age. The drainage angle of the eye becomes less efficient over time, and pressure within the eye gradually increases, which can damage the optic nerve. In some patients, the optic nerve becomes sensitive even to normal eye pressure and is at risk for damage. Treatment is necessary to prevent further vision loss.
Typically, open-angle glaucoma has no symptoms in its early stages and vision remains normal. As the optic nerve becomes more damaged, blank spots begin to appear in the field of vision. You typically won't notice these blank spots in your day-to-day activities until the optic nerve is significantly damaged and these spots become large. If all the optic nerve fibers die, blindness results.
Closed-angle glaucoma: Some eyes are formed with the iris (the colored part of the eye) too close to the drainage angle. In these eyes, which are often small and farsighted, the iris can be sucked into the drainage angle and block it completely. Since the fluid cannot exit the eye, pressure inside the eye builds rapidly and causes an acute closed-angle attack.
Symptoms may include:
· blurred vision;
· severe eye pain;
· headache;
· rainbow-colored halos around lights
· nausea and vomiting
This is a true eye emergency. If you have any of these symptoms, call your ophthalmologist immediately. Unless this type of glaucoma is treated quickly, blindness can result.
Unfortunately, two-thirds of those with closed-angle glaucoma develop it slowly without any symptoms prior to an attack.
Who is at risk for glaucoma?
Your ophthalmologist considers many kinds of information to determine your risk for developing the disease.
The most important risk factors include:
· age;
· elevated eye pressure;
· family history of glaucoma;
· African or Spanish-American ancestry;
· farsightedness or nearsightedness;
· past eye injuries;
· thinner central corneal thickness;
Your ophthalmologist will weigh all of these factors before deciding whether you need treatment for glaucoma, or whether you should be monitored closely as a glaucoma suspect. This means your risk of developing glaucoma is higher than normal, and you need to have regular examinations to detect the early signs of damage to the optic nerve.
How is glaucoma detected?
Regular eye examinations by your ophthalmologist are the best way to detect glaucoma. A glaucoma screening that checks only the pressure of the eye is not sufficient to determine if you have glaucoma. The only sure way to detect glaucoma is to have a complete eye examination.
How is glaucoma detected?
Regular eye examinations by your ophthalmologist are the best way to detect glaucoma. A glaucoma screening that checks only the pressure of the eye is not sufficient to determine if you have glaucoma. The only sure way to detect glaucoma is to have a complete eye examination.
During your glaucoma evaluation, your ophthalmologist will:
· measure your intraocular pressure (tonometry);
· inspect the drainage angle of your eye (gonioscopy);
· evaluate whether or not there is any optic nerve damage (ophthalmoscopy);
· test the peripheral vision of each eye (visual field testing, or perimetry).
Photography of the optic nerve or other computerized imaging may be recommended. Some of these tests may not be necessary for everyone. These tests may need to be repeated on a regular basis to monitor any changes in your condition.
How is glaucoma treated?
As a rule, damage caused by glaucoma cannot be reversed. Eye drops, laser surgery and surgery in the operating room are used to help prevent further damage. In some cases, oral medications also may be prescribed. With any type of glaucoma, periodic examinations are very important to prevent vision loss. Because glaucoma can progress without your knowledge, adjustments to your treatment may be necessary from time to time.
Medications
Glaucoma is usually controlled with eye drops taken daily. These medications lower eye pressure, either
by decreasing the amount of aqueous fluid produced within the eye or by improving the flow through the
drainage angle.
Never change or stop taking your medications without consulting your ophthalmologist. If you are about to run out of your medication, ask your ophthalmologist if you should have your prescription refilled. Glaucoma medications can preserve your vision, but they also may produce side effects. You should notify your ophthalmologist if you think you may be experiencing side effects.
Some eye drops may cause:
· a stinging or itching sensation;
· red eyes or redness of the skin surrounding the eyes;
· changes in pulse and heartbeat;
· changes in energy level;
· changes in breathing (especially with asthma or emphysema);
· dry mouth;
· changes in sense of taste;
· headaches;
· blurred vision;
· Change in eye color.
All medications can have side effects or can interact with other medications. Therefore, it is important that you make a list of the medications you regularly take and share this list with each doctor you see.
Laser Surgery
Laser surgery treatments may be recommended for different types of glaucoma.
In open-angle glaucoma, the drain itself is treated. The laser is used to modify the drain (trabeculoplasty) to help control eye pressure.
In closed-angle glaucoma, the laser creates a hole in the iris (iridotomy) to improve the flow of aqueous fluid to the drain.
Laser for prevention of narrow angle glaucoma or Laser iridotomy
Surgery in the Operating Room
when surgery in the operating room is needed to treat glaucoma, your ophthalmologist uses fine, microsurgical
instruments to create a new drainage channel for the aqueous fluid to leave the eye. Surgery is recommended
if your ophthalmologist feels it is necessary to prevent further damage to the optic nerve. As with laser
surgery, surgery in the operating room is typically an outpatient procedure.
What is your part in treatment?
Treatment for glaucoma requires teamwork between you and your doctor. Your ophthalmologist can prescribe treatment for glaucoma, but only you can make sure that you follow your doctor's instructions and take your eye drops. Once you are taking medications for glaucoma, your ophthalmologist will want to see you more frequently. Typically, you can expect to visit your ophthalmologist every three to four months. This will vary depending on your treatment needs.
Loss of vision can be prevented
Regular medical eye exams may help prevent unnecessary vision loss. Recommended intervals for eye exams are:
· Age 20-29: Individuals of African descent or with a family history of glaucoma should have an eye examination every three to five years. Others should have an eye exam at least once during this period.
· Age 30 -39: Individuals of African descent or with a family history of glaucoma should have an eye examination every two to four years. Others should have an eye exam at least twice during this period.
· Age 40-64: Every two to four years.
· Age 65 or older: Every one to two years.
Narrow Angle Glaucoma and Treatment
A Laser peripheral iridotomy (PI) is performed for patients with narrow angles, narrow angle glaucoma, or acute angle closure glaucoma. Aqueous fluid, the liquid that keeps the eye inflated, is made in the ciliary body of the eye, which is anatomically situated behind the iris. The aqueous fluid primarily escapes the eye by flowing between the lens and iris of the eye, and then drains via the trabecular meshwork, which is located in the angle of the eye (where the front clear cornea meets the iris, essentially). If the flow of aqueous fluid to the drainage angle (trabecular meshwork) is obstructed by a forwardly bowed iris, the patient is said to have narrow angles. This condition may predispose one to an acute episode of angle closure glaucoma. If the angles are never acutely closed, but glaucoma is still present, the patient is diagnosed with narrow angle glaucoma.
Laser peripheral iridotomy involves creating a tiny opening in the peripheral iris, allowing aqueous fluid to flow from behind the iris directly to the anterior chamber of the eye. This typically results in resolution of the forwardly bowed iris and thereby an opening up of the angle of the eye. The narrow or closed angle thus becomes an open angle.
The laser peripheral iridotomy procedure is usually completed in the laser office as a brief outpatient procedure. Prior to the procedure, the pupil is often constricted with an eye drop medication known as pilocarpine. This eye drop can cause a slight headache for a few hours. The procedure itself is completed with the patient seated at the laser, and requires no sedation. Usually, a lens is placed on the eye after topical anesthetic drops are applied to better control the laser beam. The entire procedure only takes a few minutes. The lens is then removed from the eye, and vision will quickly return to normal. After the procedure, your eye surgeon may recommend anti-inflammatory eye drop medications for the next few days. A post-op visit will be scheduled.
Does laser peripheral iridotomy reverse glaucoma?
In general, glaucoma is not reversed by any procedure or medicine. The goal of treatment is either prophylaxis against the development of glaucoma or treatment of existing glaucoma. In either case, if an ophthalmologist recommends a laser peripheral iridotomy, he or she believes this procedure is appropriate for the prevention of, or treatment of, glaucoma.
Is the procedure painful?
The surface of the eye is numbed with topical anesthetics for this procedure, but the iris is not numbed for the procedure. Therefore, when the laser beam hits the iris to create the peripheral iridotomy, mild discomfort may occur. In general, only a few very brief episodes of slight discomfort are associated with this procedure.
What are the potential complications?
A laser peripheral iridotomy is an extraordinarily safe procedure. Complications, fortunately, are very rare. These potential complications include bleeding in the eye, inflammation in the eye, and transient pressure elevations. As such, most ophthalmologists will treat the patient with eye drop medications (following the procedure) to prevent these potential complications.





